Blood glucose
-
What is blood glucose?
-
The need for glucose
-
Glucose storage
-
Effect of high/low glucose levels
<
>
|
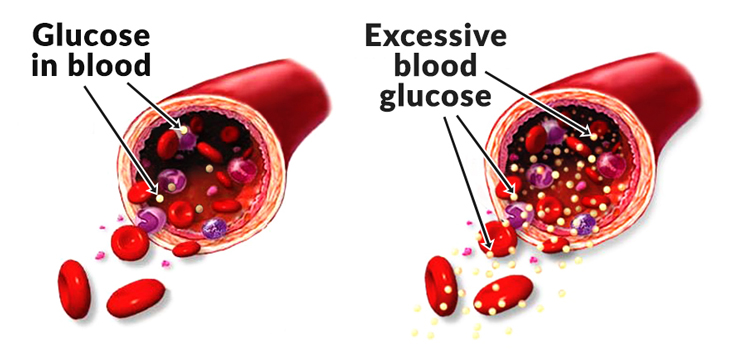
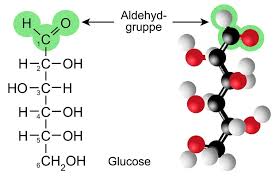
Glucose is a molecule that is essential for all living things to undergo respiration.
Respiration is the process where ATP (energy) is released from the glucose found in food. Without glucose, energy cannot be made available for living things to carry out their life processes, and they will die! Blood-glucose is the amount of glucose found in one's blood-stream. If the level of glucose in the blood is too high, this can cause problems (discussed later). If the level is too low, this means the organism won't have enough ATP to carry out its life processes. The blood-glucose level of an individual must be at a level where it is not too high or too low, and the body has ways of making this happen. |
Blood-glucose levels guide:
Set point - 4.4 to 8.0 mmol/L
Slightly low - 3.0 to 4.4 mmol/L
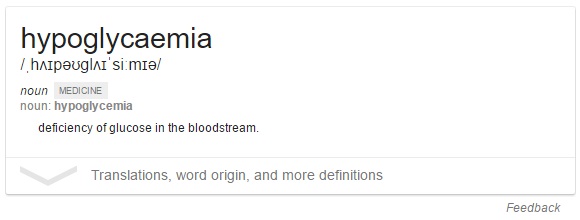
Too low (hypoglycaemic) - < 3.0 mmol/L
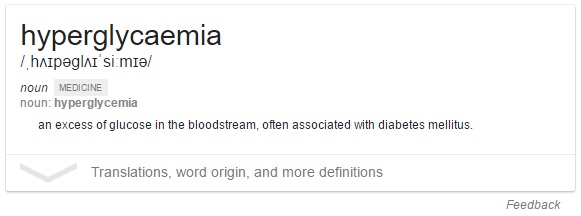
Too high (hyperglycaemic) - >8.0 mmol/L
Slightly low - 3.0 to 4.4 mmol/L
Too low (hypoglycaemic) - < 3.0 mmol/L
Too high (hyperglycaemic) - >8.0 mmol/L
The need is continuous, the supply is intermittent
We only have 3 main meals a day, and some of us will have some snacks in-between. Regardless, we are only putting glucose into our bodies (by eating carbohydrates) every couple of hours, not all the time. We are supplying our bodies with glucose intermittently. However, our body needs energy all the time, and therefore needs glucose all the time (in order for respiration to occur to get the energy)! So how does our body turn an intermittent supply of glucose into a continuous stream?
The body has two storehouses:
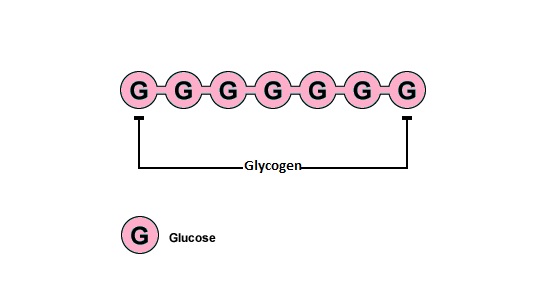
To be able to store glucose, it must be converted into something a little bit different - glucose in its original form cannot be stored by the body.
- The liver
- Skeletal muscles
To be able to store glucose, it must be converted into something a little bit different - glucose in its original form cannot be stored by the body.
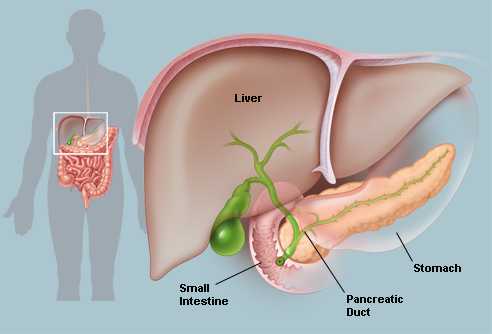
- After a meal, the glucose enters the blood and heads to the liver - here it is removed by the liver cells and converted into glycogen (the animal equivalent of starch in plants). As glycogen, glucose can be stored - removing the glucose from the blood stream. When glucose is needed, glycogen is then simply converted back into glucose which re-enters the bloodstream and is delivered to the cells where it will be used in respiration.
- Our muscles are the places in our body which require the most glucose (as our muscles need lots of ATP as they do so much work!), and when they run out of lgucose they need an immediate replenishment. Therefore, our body will store glucose in our muscles (as glycogen). During vigorous exercise, the glycogen is converted to glucose and used to make ATP. During muscle recovery, these glycogen stores are topped up using blood-glucose (which is why it is good to eat after exercise).
|
So, in simple terms, the body receives an input of glucose (food) and breaks it down (digestion. It then absorbs it into the blood stream via the intestines, and it heads to the liver. Here it can be converted into glycogen, allowing the body to store the glucose (as glucose the body just uses it up, but when made into the glycogen the body can't use it up).
If we are eating properly, we have plenty of glucose to store. As the day goes by, and as we need energy, our body can just convert that glycogen back into glucose which can then be used in respiration, to make ATP, to keep our cells (and therefore us) functioning properly! |
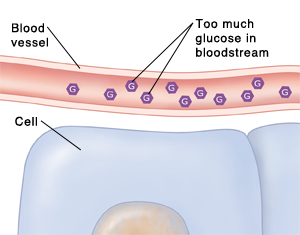
Effect of high BG levels |
Effect of low BG levels |
|
|
Blood-glucose regulation in humans
1.Environmental change detected by glucose receptors in the pancreas
|
2.In the pancreas are the islets of langerhans, the control centre, which co-ordinates an appropriate response
|
3.Depending on the type of response needed, the effectors will kick into action. These are the alpha and beta cells, found in the islets of langerhans
|
Blood-glucose levels are regulated completely by the endocrine system and completely by the pancreas.
Pancreas
-
The pancreas
-
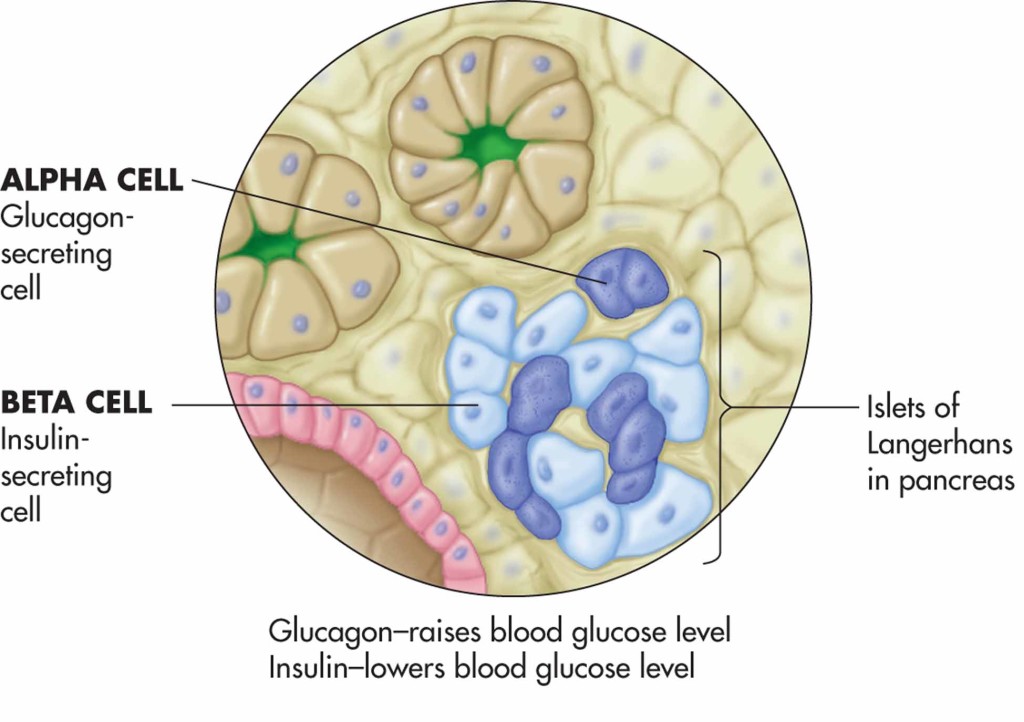
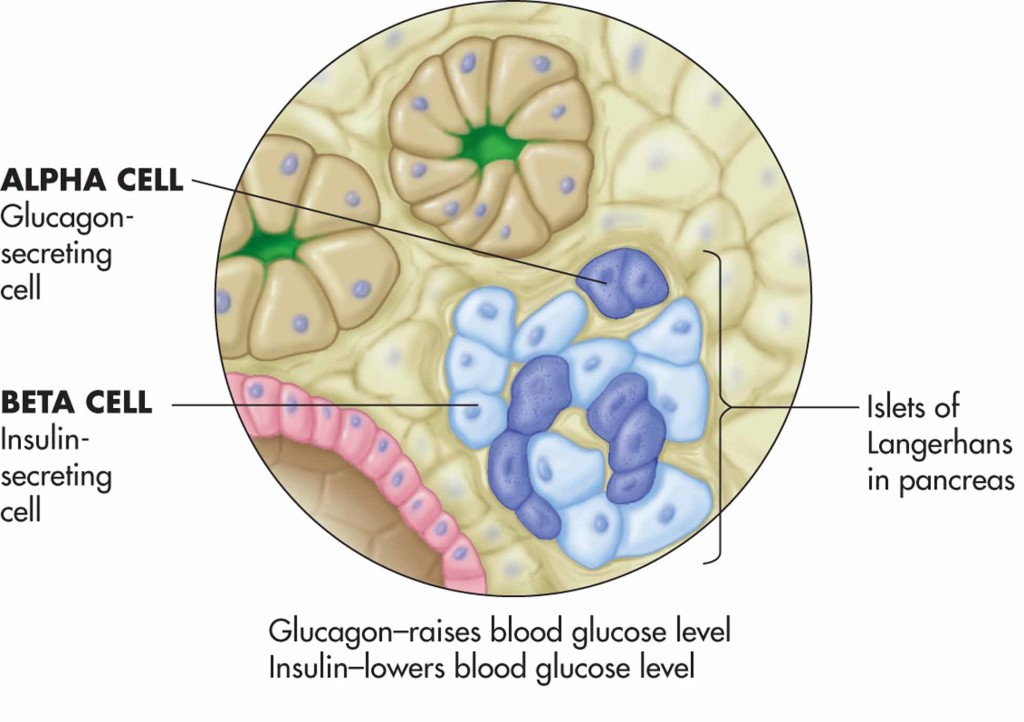
Islets of Langerhans
-
Alpha cells
-
Beta cells
<
>
Blood-glucose levels are completely reliant on the pancreas for the detection of any disruption, the co-ordination of an appropriate response and the carrying-out of the response. All these roles are performed by the pancreas.
Within the pancreas are specialized glucose-receptor cells which detect fluctuations in blood-glucose level and can co-ordinate the response required to return the BG level to within the normal range.
Within the pancreas are specialized glucose-receptor cells which detect fluctuations in blood-glucose level and can co-ordinate the response required to return the BG level to within the normal range.
The islets of langerhans are little clusters of cells that control the blood-glucose levels within the blood stream. Many of the other cells in the pancreas are designed to make and secrete digestive enzymes into the stomach. The cells we're interested in are the alpha and beta cells, found in the islets, and they increase/decrease BG levels.
|
When stimulated, beta cells:
Increased amounts of glucagon (secreted by alpha cells) in the blood stream also stimulates the release of insulin from the beta cells. Insulin inhibits glucagon, so when blood glucose levels are near the set point, glucagon will be inhibited and stop converting glycogen into glucose (otherwise the BG levels will get too high!) |
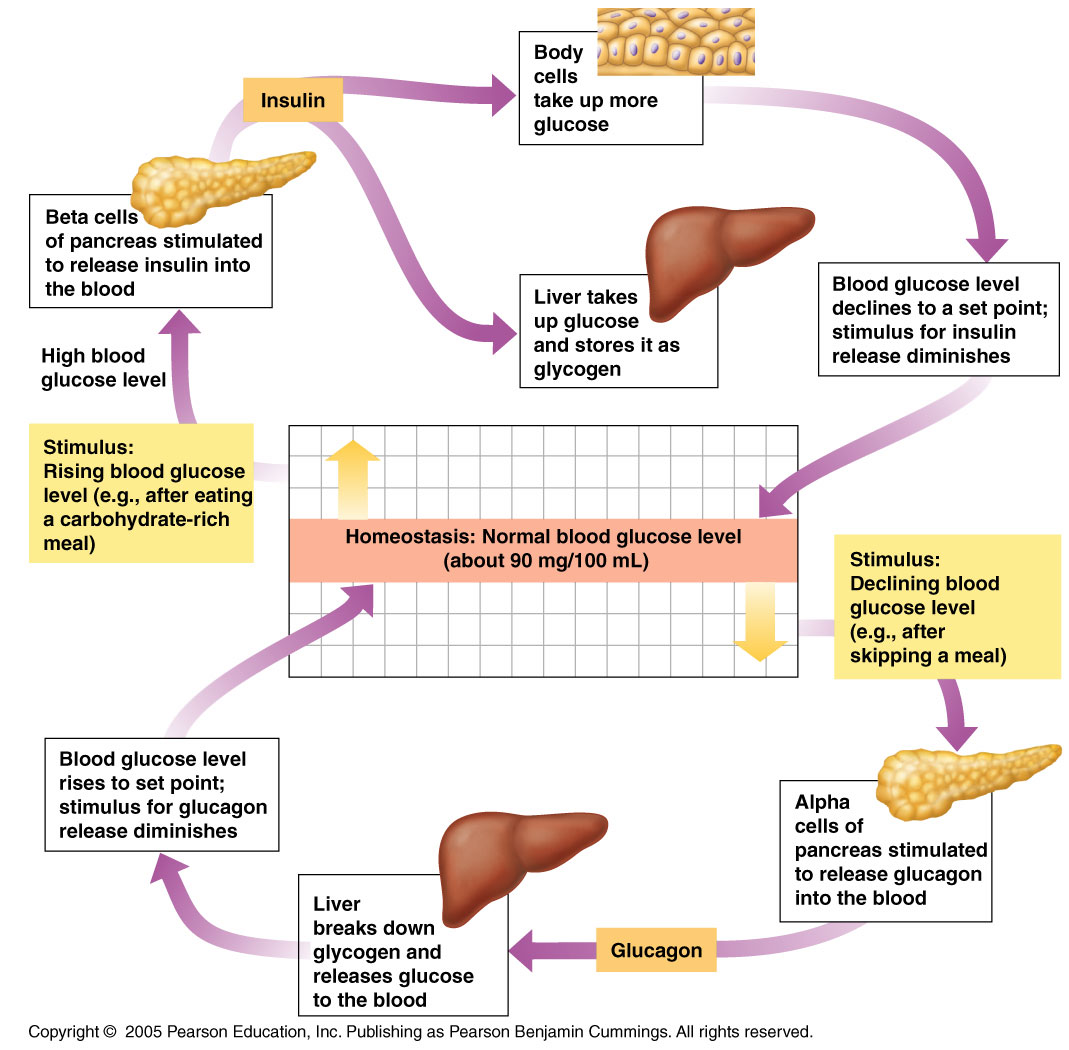
Disruptions frequently occur within this system - when our blood glucose levels get low (hypoglycaemia) or too high (hyperglycaemia) - these disruptions can be fixed through the homeostasis response system - a negative feedback loop.
Counteracting hypoglycaemia
You may experience hypoglycaemia when...
|
When your BG level drops below the set point (either from lack of glucose input (eating) or the using up of glucose for increased respiration (to get more ATP energy), your body will respond by trying to increase the number of glucose molecules in your blood stream. The glucose receptors in the pancreas detect the drop in blood-glucose concentration. Almost intuitively, the islets of langerhans co-ordinate an appropriate response by activating the appropriate cells. In this case, to increase blood-glucose level, the alpha cells get to work.
|
Response:
|
Counteracting hyperglycaemia
You may experience hyperglycaemia when...
You eat some food - particularly a large meal or one high in sugar
|
When your BG level rises above the set point, your body will respond by trying to reduce the number of glucose molecules in your blood stream. The glucose receptors in the pancreas detect the increase in blood-glucose concentration. Almost intuitively, the islets of langerhans co-ordinate an appropriate response by activating the appropriate cells. In this case, to decrease blood-glucose level, the beta cells get to work.
|
Response
Beta cells release insulin (a hormone) |
- Insulin stimulates the uptake of glucose by other cells in the body (to try reduce the concentration of glucose in the blood) - Insulin causes glucose to be converted into glycogen by the liver (reducing blood-glucose concentration) |
Blood-glucose levels return to normal |
Restored glucose levels signal to receptor cells that response is no longer necessary. Beta cells stop releasing insulin. This is negative feedback. |
Possible breakdowns
When the body cannot restore BG levels back to equilibrium without help
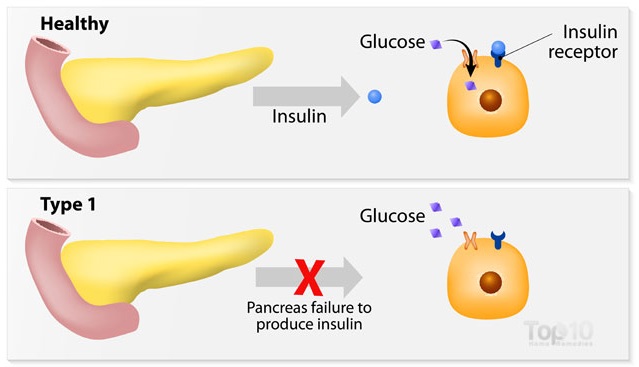
Type 1 Diabetes
-
Causes
-
Symptoms
-
Treatment
-
Risk factors
<
>
|
Type 1 diabetes is caused most frequently by an auto-immune condition where the body's cells attack the beta cells. When the beta cells are damaged, they cannot make insulin - so when you eat sugar, your body is unable to effectively process and deal with all that sugar. Various factors may contribute to type 1 diabetes, including genetics (the condition is inheritable - the beta cells are impaired from birth) or exposure to certain viruses (which cause the autoimmune disorder leading to diabetes) |
Some of the symptoms of Type 1 diabetes include:
- Thirst
- Passing more urine
- Weight loss
- Very tired
- Mood changes
- Abdominal pain, nausea, vomiting
- Skin infections, thrush
- Extreme hunger
- Poor concentration and performance
- People with Type 1 diabetes need to closely monitor their blood-glucose levels. This must be done several times a day. At specific times of the day, they must inject themselves with insulin.
- More recently, insulin pumps have been attached to Type 1 diabetics and this automatically reads their BG levels and administers the right dosage of insulin.
- Eating a healthy diet where the carbohydrates are spread throughout the day and not eaten all at one meal (carbohydrates are glucose-rich foods).
- Exercising frequently helps the body to use insulin more effectively and this is recommended.
There are many risk factors:
- Family history - anyone who has siblings or parents with the condition will have an increased risk of getting Type 1 diabetes themselves
- Genetics - some genes increase the risk of getting Type 1 diabetes
- Geography - evidence shows that the further away from the equator you live, the more people in your area have Type 1 diabetes.
- Age - Type 1 diabetes can begin at any age, but more likely during 4-7 years old, and again between 10-14 years old.
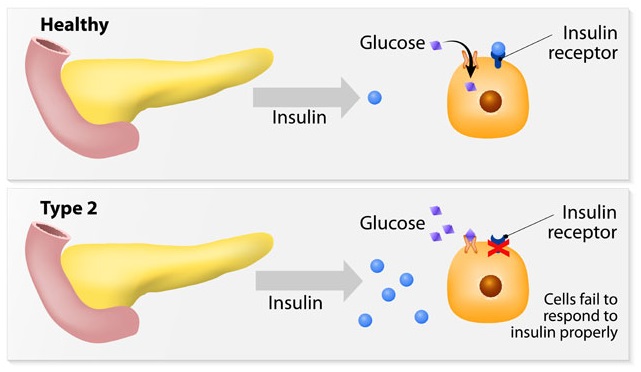
Type 2 Diabetes
-
Causes
-
Symptoms
-
Treatment
-
Risk factors
<
>
|
Some of the symptoms of Type 2 diabetes include:
- Lacking energy, feeling tired
- Feeling thirsty
- Going to the toilet quite often
- Getting infections frequently
- Getting infections that are difficult/slow to heal
- Poor eyesight or blurred vision
- Often feeling hungry
Type 2 diabetes can be managed if you follow the treatment recommended to you by your doctor. Three things you need to keep in consideration:
All three things will help reduce the symptoms of Type 2 diabetes. The goal of these things is to lower the level of blood-glucose and help your body to use its insulin more effectively over time. You may need to manage your diabetes with insulin as well as the above three things, if necessary. Medication may also be recommended.
- A healthy diet
- Exercise
- Weight loss
All three things will help reduce the symptoms of Type 2 diabetes. The goal of these things is to lower the level of blood-glucose and help your body to use its insulin more effectively over time. You may need to manage your diabetes with insulin as well as the above three things, if necessary. Medication may also be recommended.
You're more likely to get Type 2 Diabetes if you:
- Are European and 40 years of age or older
- Have diabetes in your family (grandparents, parents, brothers or sisters)
- Are Maori, Asian, Middle Eastern or Pacific Island descent aged 30 years or older
- Have high blood pressure
- Are overweight (especially if you carry most of your weight around your waist)
- Have been diagnosed as having pre-diabetes (also known as impaired glucose tolerance) - this occurs when the glucose (sugar) in your blood is higher than normal, but not high enough to be called diabetes